Implant contraceptive use on the rise in Ghana – Study
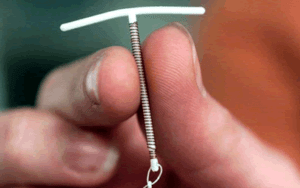 Implant contraception use is rising rapidly and equitably in many sub-Saharan African (SSA) countries including Ghana, across almost all socio-demographic categories, a study says.
Implant contraception use is rising rapidly and equitably in many sub-Saharan African (SSA) countries including Ghana, across almost all socio-demographic categories, a study says.
It indicates that Ghana has a contraceptive prevalence rate (CPR) of 25 per cent from 2016 – translating into one-out-of-four married women using family planning methods.
It however moved from 5.1 to 8.1 per cent in the use of implant.
The family planning method device with its gains is exceeding the combined increases for other methods like the IUDs (Intrauterine device), pills, condoms and injectables.
Though injectables are the preferred method, the use of implants was increasing among married, sexually active unmarried women, nulliparous and breastfeeding women in the majority of the 12 countries sampled including Ghana in the study.
Kenya however tops the global pack as its population is identified as having stepped up the use of implant contraceptive, the report outlines.
The study, “Liftoff: The Blossoming of Contraceptive Implant Use in Africa,” is a programmatic review and analysis of Global Health: Science and Practice campaign.
It was launched at the General Annual Meeting of the Reproductive Health Supplies Coalition (RHSC) in Brussels, Belgium, on March 22, this year.
The study draws from two sources of representative national population data, Demographic and Health Surveys (DHS) and Performance Monitoring and Accountability 2020 (PMA2020) surveys in 12 SSA countries including Nigeria, Burkina Faso, DRC, Ethiopia, Malawi, Niger, Senegal, Tanzania, Uganda, Zimbabwe, Kenya and Ghana. The countries were sampled in at least a recent survey published between 2015-2017 and two prior surveys from 2003-2014.
Dr Roy Jacobstein, Senior Medical Advisor, IntraHealth and lead researcher, in an email said “Implant CPR in SSA was only 1.1 per cent but conscious price reductions, much-increased commodity supply, greater government commitment to rights-based family planning, broader WHO eligibility guidance, and wider adoption of high-impact service delivery practices have resulted in expanded client access and marked increases in the device prevalence and share of the method mix.“
“Ten of the 12 countries now have an implant CPR around 6 per cent or higher, with three countries above 11 per cent. Increased implant use has been the main driver of the increased mCPR attained by 11 countries, with gains in implant use alone exceeding combined gains in use of injectables, pills, and intrauterine devices.”
Overall contraceptive use is higher in East and Southern Africa than West Africa. In countries as diverse as Burkina Faso and Ethiopia, the Democratic Republic of the Congo and Ghana, Kenya and Senegal, implant use now accounts for one-fourth to one-half of all modern method use.
Implants have become the first or second most widely used method in 10 countries. In the seven countries with multiple surveys conducted over a two to three-year span between 2013–14 and 2016–17, average annual gains in implant prevalence range from 0.97 to 4.15 percentage points; this contrasts to historical annual gains in use of all modern methods of 0.70 percentage points in 42 SSA countries from 1986 to 2008.
Kenya has a CPR of 59.9 per cent but Ghana is 5.9 per cent in the use of implants, Tanzania 6.7 per cent, Uganda 7.1 per cent, Senegal 7.1 per cent, Ethiopia 8.3 per cent, Zimbabwe 9.6 per cent, Malawi 11.5 per cent and Burkina Faso 11.8 per cent.
Kenya has the highest prevalence rate globally which meant that sexually active populations are having protected sex and did not want to get pregnant by bouts of sex.
According to the study, the rise in usage is facilitated by service delivery by International NGOs assisting governments and the private sector to provide contraceptive services at the right time and at the point of need.
Attributions of Implant
The factors underpinning the increases in implants usage in SSA includes ease of provision, convenient and duration of action, effectiveness, uncomplicated provision, ready reversibility, prompt action to fertility, suitability to all reproductive intentions, high client satisfaction and continuation as well as less demanding on health system infrastructure.
Almost 26 million implant devices have been supplied to SSA countries between 2013 and 2017 at a savings of over $230 million.
Public, private participation in the supply chain has led to marked reduction in commodity cost, the sine qua non of increased implant availability and access and use. A lowered implant commodity cost of $6.90 – $8.0 per set is assured through at least 2023, the study anticipates.
The study challenges major actors to make implant removal services routinely and regularly available and affordable on a wide scale as well as make the commodity free and highly subsidized for the disadvantaged and the poor in society.
It stated that implant device offers a major success story for family planning methods due to the increase in access and use in a rapid, substantial and generally equitable manner, even under culturally diverse and varied geographical widespread and economically deficient and programmatically different country contexts.
By Maxwell Awumah, back from Brussels, Belgium
